What is the Connection Between Rheumatoid Arthritis and Acne
Dec 21, 2023
You probably know rheumatoid arthritis, often RA is an autoimmune or inflammatory disease. It means your immune system has gone crazy, attacking your joints in error. Nonetheless, RA is a systemic illness, as with many inflammatory arthritis disorders.
It indicates that your overactive immune system can potentially harm other parts of your body, including your skin. Certain skin issues are more significant than others, and they can be brought on either by rheumatoid arthritis (RA) condition itself or by the drugs taken to treat it.
It's may that you don't have any problems at all with your skin. According to the study, only 26% of RA patients exhibit some form of skin alteration. However, even if it only affects a small percentage of RA patients, those who suffer from skin issues are more likely to develop severe forms of the disease.

Arthritis-Related Skin Problems
Hidradenitis Suppurative
Acne inverse is a common name for hidradenitis suppurative (HS), an inflammatory skin disorder. It begins as a series of little bumps on the skin, similar to pimples, and can progress to larger, more painful lesions or boils.
Clogged hair follicles or sweat glands are a common cause of this problem, manifesting in areas of the body where the skin is directly in contact with itself. According to recent studies, people with RA have a higher chance of developing HS, and certain persons with HS have a higher risk of acquiring RA.
Rheumatoid Vasculitis
The inflammation that occurs with RA can also affect the blood vessels. Rheumatoid vasculitis (RV) is a form of this, although fortunately, it only affects 1% of RA patients. A red or purple rash will often appear on your legs.
Large ulcers on the legs and fingers, purple lesions, and other skin sores are symptoms of the most severe form of this condition. Muscle weakness, chest discomfort, and tingling/numbness in the fingers and toes are some symptoms that may occur if RV has spread to other sections of the body.
Eventually, RV can lead to potentially fatal consequences, including strokes and heart attacks. You should consult a doctor immediately if you see any rash, particularly purple lumps or sores. A dermatologist will do a biopsy to confirm whether or not the lesion is RV.
Whether or whether the disease is prevalent determines the course of treatment. Doctors may prescribe steroids if it's localized (in your fingers). Treatment with an immunosuppressant, such as methotrexate or intravenous infusions of rituximab, is recommended for those with more severe symptoms (such as leg ulcers and chest pains).
Neutrophilic Dermatosis
Neutrophilic dermatosis is uncommon and often only occurs in people with advanced illnesses. A little under one percent of individuals have these skin disorders in RA. While women are more likely to be affected than males, it still affects a disproportionate number of people.
The rashes of various forms share large numbers of white blood cells (neutrophils) without evidence of infection. Plaques, or elevated areas of skin, can appear anywhere on the body, including the face, chest, legs, and arms. The cut on your lower thigh might be huge and inflamed, or you could have a rash that won't disappear.
These wounds might be purple-raised lumps, or they could have pus. Surprisingly, neutrophilic dermatosis can clear up independently but can also spread to other body regions, including the eyes. This rage and inflammation can spread and eventually lead to tissue death at the wound's margins.
Rheumatoid Nodules
Rheumatoid nodules develop in around a quarter of RA patients. Only those whose blood tests for rheumatoid factor or anti-CCP (cyclic citrullinated peptide) antibodies will develop these nodules. One protein your immune system can make is called rheumatoid factor.
It's linked to inflammation, which may wreak havoc on your body, particularly the lining of your joints. Most rheumatoid nodules are between a few millimeters and a few centimeters in diameter, most commonly affecting Caucasian guys.
Typically, they manifest on pressure points, such as the fingers and heels, and the arms' extensor surface (the region outside a joint) around the elbow. Nodules of rheumatoid arthritis have been seen in the lungs.
Skin Sensitivity And Bruising
Common complaints of patients include easy bruising, which is often attributable to the use of drugs that raise blood pressure and produce thrombocytopenia (a condition characterized by a deficiency of platelets). Platelet counts can decline after taking certain medications, including methotrexate and certain biologics, and steroids, especially in elderly patients who have been taking them for a time.
Because your skin is more delicate, you will easily bruise and be more vulnerable to minor injuries. Also, the skin is typically quite dry. Swelling of the fingers can cause the skin to become tight and thin, making them more susceptible to bruising, and in rare cases, ridges can even appear in the nails.
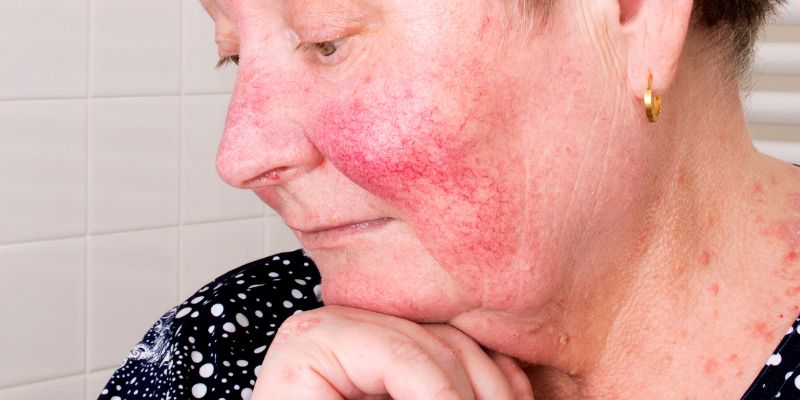
Granulomatous Dermatitis
Granulomatous dermatitis is a type of rash that looks like plaques and can be itchy and unpleasant. While it most frequently manifests on the trunk and the inside surfaces of the thighs, this condition can manifest itself anywhere on the body. This rare disorder often only manifests in individuals with advanced RA with positive rheumatoid factor tests.
Conclusion:
Although there is little research on the subject, rheumatoid arthritis (RA) does not seem to contribute to acne. A conclusion cannot be made at this time without more study. However, rheumatoid arthritis is linked to other skin disorders, such as rheumatoid vasculitis. See your doctor if you notice any changes to your skin after being diagnosed with RA.
Whether or not you have rheumatoid arthritis or are dealing with acne, it's advisable to consult a doctor about what will work best for you. Treatments, both topical and oral, are readily accessible. Habits of good skincare and lifestyle, such as frequent face washing and stress management, can also aid.